Families are often confused, upset and even frightened by their loved one’s new and often challenging behaviors associated with the progression of Alzheimer’s or related dementias. As symptoms progress, a myriad of changes can occur:
- People with Alzheimer’s and related dementias have a lower threshold to stress and stimulation
- Control of certain functions such as perception begins to change
- People often lose inhibition
- They can experience an altered state of reality and could show signs of aggression, paranoia, hallucinations, irritability or anxiety
- Information that was once readily perceived, interpreted, understood and acted upon may become unreliable
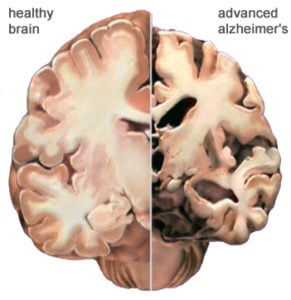
The first line of defense in managing challenging behaviors is taking a behavioral approach, rather than relying on medications.
Here are some tips to help you or a loved one cope with the challenging behaviors brought on by dementia:
Maintain structure, consistency and daily routines, as it allows for feelings of fulfillment and success for both the person with dementia and their caregivers when navigating the day-to-day.
Prevent frustration. Watch for signs of over-stimulation or confusion. Avoid loud noises and clutter. Turn off the television if you want to have a conversation, and try to phrase questions so they may be answered simply. Distraction can be a very effective approach to managing challenges. For example, if they are having trouble putting on a sweater, redirect to something else and then try again after some time has passed.
Avoid confrontation. Do not argue or try to reason if presented with a challenging behavior. Even if your family member is yelling or criticizing you, avoid expressing anger or impatience in return. Try softening or quieting your tone. Fatigue is the most common denominator in outbursts – both for the person with Alzheimer’s and the caregivers!

Be positive. Use positive expressions and humor when appropriate to diffuse tense situations. Remain calm. Use a gentle touch to reassure (if the person is willing to accept it). Build periods of relaxation into the daily routine, such as sitting in a rocking chair or favorite recliner with a cup of tea.
Dealing with hallucinations. If your loved one is hallucinating that they had a conversation with a deceased family member, but this was a pleasant experience for them, go along with their reality. However, if the hallucination (or any behavior) causes fear and distress, it is vital to request a medical evaluation. Difficult behaviors that persist or have the potential to cause harm need to be attended to by a skilled and knowledgeable physician.
For more tips, use these online resources:
Understanding an Alzheimer’s Diagnosis
Help with Communication and Behavior
Communicating with Someone with Dementia
Alzheimer’s Care: Practical tips
Support: Message Boards
Caregiver Support Groups


 Tadd Clelland
Tadd Clelland